The Dark Side of Birth Control: What You Need to Know
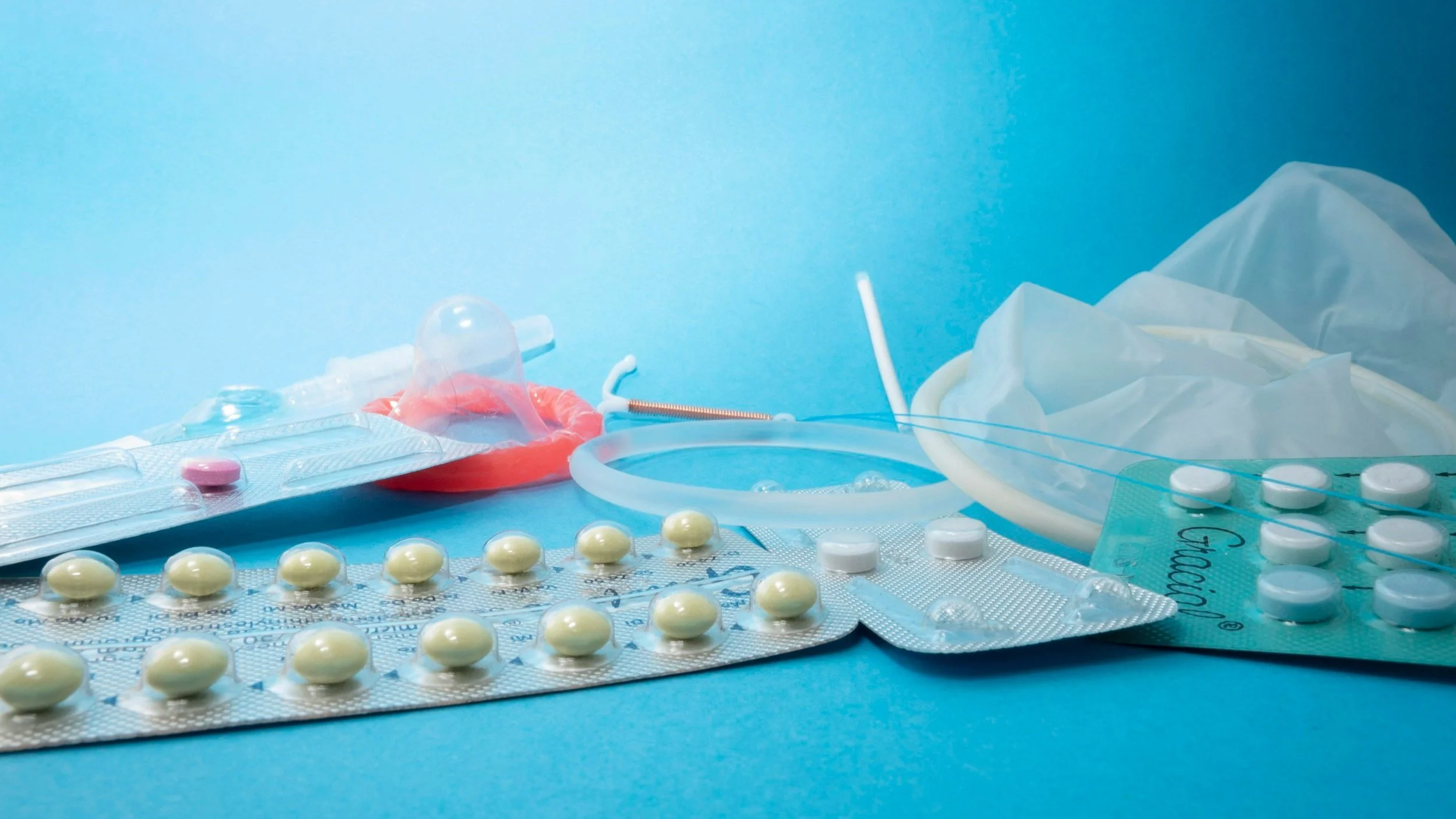
*If you are on hormonal birth control your body will not go through the natural menstrual cycle phases. If once a month you do “bleed” it is defined as a medically induced bleed. The withdrawal bleed is caused by a drop in hormone levels, not by the natural hormonal fluctuations that occur during a typical menstrual cycle. Since ovulation is suppressed, there is no egg release.*
The information here is a summary of countless hours of studies, podcasts, documents, and videos I have sourced. I highly suggest looking at the sources provided as well as doing your own research. I also ask you go into this with an open mind and ready to learn because it is one of the most important pieces of information I could give you.
A history lesson on birth control:
In 1960, the first oral contraceptive pill was approved by the Food and Drug Administration (FDA). Once released, pharmaceutical companies realized that birth control pills represented a potentially long-term product. By introducing birth control pills that needed to be taken every day, they ensured a consistent, ongoing market. This sparked the question: what else can we make that someone can consume their entire life?
Birth control pills could be marketed towards women from their early teens to mid-40’s, creating a long-term customer base. This was highly appealing to pharmaceutical companies, as it meant patients could be on a medication for several decades, leading to consistent profits. The success of the pill encouraged companies to expand their focus to other drugs for chronic use, paving the way for the development of medications for conditions like high blood pressure, cholesterol, mental health disorders, diabetes, and more.
An Overview:
Birth control pills and other hormonal contraceptives use synthetic versions of naturally occurring hormones in the body to prevent pregnancy by regulating or inhibiting ovulation, thickening cervical mucus, and altering the uterine lining.
Progestin (synthetic progesterone)- Progestin is a synthetic version of progesterone, a hormone naturally produced by the ovaries. It plays a crucial role in regulating the menstrual cycle and maintaining pregnancy. In birth control, progestin works in several ways:
It prevents ovulation so no fertilization can occur, it thickens cervical mucus, making it harder for sperm to enter the uterus and reach an egg, and it thins the uterine lining reducing the chance of a fertilized egg implanting. There are several types of progestins used in birth control: Levonorgestrel (found in many birth control pills, IUDs, and emergency contraception) Norethindrone (used in various forms of hormonal contraception), Desogestrel (common in some combination birth control pills), Drospirenone (often combined with estrogen in pills like Yaz).
Ethinyl estradiol (synthetic estrogen)- Ethinyl estradiol is a synthetic form of estrogen, the primary female sex hormone responsible for regulating the menstrual cycle. In birth control, estrogen helps enhance the suppression of ovulation, contributing to the effectiveness of the contraceptive by preventing egg release. Another common form of synthetic estrogen seen is estradiol valerate, this is a form of estradiol (the natural estrogen found in the body) that is used in some birth control pills. It's often found in newer, lower-dose contraceptives and is considered to have a closer chemical structure to the natural hormone. Lastly, mestranol, this is a synthetic estrogen that was used in older birth control pills but has largely been replaced by ethinyl estradiol due to its higher potency and effectiveness.
Other Forms of Hormonal Birth Control:
Injections
(Like Depo-Provera) – These deliver medroxyprogesterone directly into the bloodstream, offering effective contraception for up to three months with each shot. Lawsuits are currently being filed against Pfizer, the manufacturer of Depo-Provera, due to allegations that the drug may be linked to brain tumors.
Implants
(Like Nexplanon) – A small, flexible rod inserted under the skin that releases etonogestrel over time, providing effective contraception for up to three years.
IUDs
(like Mirena) – This is an intrauterine devices that release levonorgestrel directly into the uterus, offering long-term (3-7 years), birth control.
Some facts:
- Around 65% of women aged 15-49 use birth control, according to a survey conducted from 2017 to 2019 by the Centers for Disease Control and Prevention (source)
-33% of teen girls and 14% of all U.S. women are put on birth control for nonpregnancy reasons (acne, painful periods, etc.) (source)
-1 in 5 teen girls are put on birth control, but the use of birth control before the age 19 causes a lifetime of increased risk for depression (even after they stop using birth control). It has also been shown that the first two years of OC use were associated with a 71% increased risk of depression (source)
-Women on birth control are 23% more likely to be prescribed an antidepressant, and the risk is even higher among adolescents aged 15–19: those on combined oral contraceptives are 80% more likely, and those on progestin-only pills are more than twice as likely, to receive an antidepressant prescription compared to peers not using hormonal contraception. (source)
-Women who use birth control have an increased risk of developing Crohn’s disease, with studies showing about a 24% higher risk compared to women who do not use hormonal contraception. (source)
-Birth control works at a neurological level by altering the communication between your brain and ovaries, affecting both spatial (navigation) and verbal (fluency) tasks. (source)
-Many forms of hormonal birth control are classified as Class 1 carcinogens, linked to increased risks of breast and cervical cancer. Prolonged use may also raise the risk of liver tumors. (source)
-Hormonal birth control can alter the gut microbiome, potentially affecting the balance of beneficial and harmful bacteria in the digestive system. (source)
-Hormonal birth control can deplete key nutrients, including riboflavin, B6, B12, folate, vitamin C, magnesium, selenium, and zinc—nutrients essential for mood stability, ovulation, pregnancy, immune function, and healthy blood. Without proper supplementation, these deficiencies can significantly impact your health. Selenium and zinc are particularly important for producing thyroid hormone and converting it into its active form, T3 (source)
-Yeast, specifically Candida species, is fueled by estrogen, which is why yeast infections are more common in people using hormonal birth control that raises synthetic estrogen levels. Estrogen helps maintain the balance of microorganisms in the vagina by promoting lactic acid production from lactobacilli. This lactic acid keeps the vaginal environment acidic, inhibiting the growth of harmful microbes, including yeast. Elevated estrogen also increases vaginal glycogen, providing more food for Candida and further increasing infection risk. (source)
However, when estrogen levels fluctuate, such as with hormonal contraceptive use or during the menstrual cycle, the delicate balance of microorganisms in the vaginal environment can shift. This imbalance can create conditions where yeast, particularly Candida species, may overgrow. Women using hormonal birth control are more susceptible to vaginal yeast infections due to the effects of synthetic estrogen and progestin in many forms of contraception. These hormones can alter the vaginal flora, increasing glycogen production, which in turn provides more nutrients for yeast to thrive. This hormonal influence changes the vaginal environment, making it more favorable for yeast infections to occur.
Yeast is a type of fungus, and fungi produce byproducts. One of the byproducts that the species Candida produces is ammonia. Ammonia is then released into the surrounding tissue, which can cause harm to the body and contribute to symptoms like brain fog, making it undesirable in the body.
Taking birth control containing estrogen can affect your thyroid, which regulates metabolism, energy, and mood. Estrogen increases thyroid-binding globulin (TBG), a protein that binds thyroid hormones (T3 and T4) in the bloodstream, rendering them inactive.”
When estrogen levels are elevated, such as when taking estrogen-containing birth control, more thyroid hormones get "bound" by TBG and cannot perform their functions in your body. This may lead to a condition known as subclinical hypothyroidism or low functional thyroid hormone levels. (Symptoms include fatigue, weight gain, and depression). Your thyroid hormones appear normal in blood tests, but they’re not active enough to support your body's needs.
The copper intrauterine device (IUD) is a non-hormonal contraceptive that releases small amounts of copper into the uterus. This copper is toxic to sperm, preventing fertilization, and alters the uterine environment to make it less suitable for implantation if fertilization occurs. Copper IUDs also inflame the uterus, and while the primary inflammatory response is localized within this area, some studies suggest that the inflammatory response may extend beyond the uterus, potentially affecting other parts of the body. For instance, a study observed elevated levels of interleukin-6 (IL-6), a proinflammatory cytokine, in the blood of women using a copper IUD for 10-24 months. However, it remains unclear whether this increase is due to "overspill" from the local inflammatory response or indicates systemic immune activation. (source)
Copper toxicity refers to the condition where there is an excess amount of copper in the body, which can lead to harmful effects on health. While copper is an essential trace element for various bodily functions (such as enzyme activity, iron absorption, and nervous system function), too much copper can lead to various health issues. While copper IUDs are generally safe for most people, there are some who may be more sensitive to copper or have a condition that makes them prone to copper toxicity. Some symptoms of copper toxicity include headaches, fatigue, nausea, joint pain, mental confusion, abdominal pain, and liver damage. It is also common for individuals with a copper IUD to experience increased menstrual bleeding, heavier periods, or cramping. Copper IUDs also increase the chance of bacterial vaginosis (vaginal infection caused by an imbalance in the normal bacteria found in the vagina). (source)
Nexplanon is a small, flexible rod inserted under the skin of the upper arm. The implant releases a steady amount of etonogestrel over time to prevent pregnancy (this is a 24/7 release). Nexplanon increases the risk of blood clots, strokes, ovarian cysts, liver issues, and heart attacks. It can also cause various hormonal side effects, including depression, headaches, ovarian cysts, irregular periods, or amenorrhea (absence of periods). There is also a possibility that it can move within your body and shift to an area it is not supposed to be, potentially causing serious complications. (source)
What should a normal cycle look like?
Duration: 3 to 7 days
Frequency: Cycles between 21 and 35 days
Flow: Starts light, becomes moderate to heavy, and ends light
Blood color: Bright red, dark red, brown, or even pink, depending on the stage of the period
Symptoms: Mild cramping, bloating, mood changes, headaches, and breast tenderness are common
What should it not look like?
Excessive bleeding (menorrhagia): soaking through a tampon or pad every hour for several hours, or bleeding more than 7 days consistently
Very irregular periods: cycles shorter than 21 or longer than 35 days, missing periods, or periods that skip multiple months
No period (amenorrhea): absence of periods for 3 months or longer
Severe pain (dysmenorrhea)
Sudden changes in your cycle
A clinical pearl-if you are on hormonal birth control, so is your man. Since birth control changes your vaginal mucus, and things go places, this can be absorbed and passed on.
There’s some interesting research on how hormonal birth control might influence attraction and partner selection. Studies suggest that women using hormonal contraceptives may be more attracted to men with less masculine features. Women on hormonal birth control’s sense of smell actually changes. This makes them unaffected by pheromones (a chemical substance that animals and humans release to communicate with each other, which affects human behavior). (source)
Women who are not on hormonal birth control are more likely to be attracted to men with immune systems that differ from their own, which is thought to be an evolutionary advantage for producing offspring with better immune system diversity. However, the theory is that hormonal birth control may disrupt this natural mechanism, leading women to unknowingly choose partners who might not offer the same genetic benefits in terms of immune compatibility. This could be because women on birth control are less attuned to the pheromones, including those related to testosterone, that they would otherwise respond to. (source)
Consider this…
What do you think about the idea that birth control companies might be profiting from a lifelong customer base rather than focusing on long-term solutions for women’s health?
Do you think pharmaceutical companies prioritize symptom management over finding lasting solutions for women’s health concerns?
What are the ethical implications of prescribing a medication that can create a lifelong dependency, rather than addressing the root cause of health issues?
If birth control is designed to be used over decades, do we run the risk of normalizing chronic use of a synthetic drug rather than addressing the underlying health issues?
Patches
(such as Ortho Evra or Xulane) – These release synthetic hormones (ethinyl estradiol and norelgesetromin) through the skin, it provides effective contraception for one week at a time and it replaced weekly.
Temporary Fixes, Not Solutions
A significant number of adolescent girls are prescribed birth control for non-contraceptive purposes, including the regulation of menstrual cycles, management of menstrual-related pain, treatment of endometriosis, and reduction of acne. However, it is important to recognize that hormonal birth control does not address the underlying causes of these issues. Instead, it typically masks the symptoms.
For instance, while birth control may regulate bleeding and alleviate pain, it does not resolve the root causes of menstrual irregularities or conditions such as polycystic ovary syndrome (PCOS) or endometriosis. Additionally, it does not address contributing factors such as lifestyle habits, nutrition, or stress. Similarly, while birth control can provide temporary relief for acne, it may not correct the hormonal imbalances that could be contributing to the condition.
One key concern is that when a young woman discontinues the use of birth control, the underlying health issues that were initially masked may resurface, often without having been adequately addressed. Therefore, while birth control may offer short-term symptom management, it is essential to adopt a comprehensive approach that not only manages symptoms but also identifies and treats the root causes of these health concerns through other medical or lifestyle interventions.
Taking a birth control to stop a symptom is like silencing a fire alarm during a fire. More and more individuals are prescribed medications to manage symptoms over the long term, rather than focusing on diagnosing and treating the root cause of their health concerns. Pharmaceutical companies don’t want to cure your disease, they want to treat it with something they will profit off of for your entire life. Our bodies are perfectly designed, if something is wrong, it is important to listen to the signals they send. Consider your menstrual cycle as your monthly “health report card”, a powerful indicator at your overall health. If you experience heavy, painful periods, irregular cycles, or severe cramping, these are not normal, even if they are common. Such symptoms often indicate underlying issues that require attention, which can range from lifestyle changes to more serious conditions that could affect future fertility. In some cases, poor lifestyle choices can exacerbate these issues. If you simply shut off the fire alarm, the fire isn’t going to go away. In many ways, our bodies serve as an early warning system—like a canary in a coal mine—alerting us when something needs to be addressed.
If you have been on a hormonal birth control since you were a teenager, your natural menstrual cycle may not have had the opportunity to regulate itself. The synthetic hormones in birth control suppress your body's natural hormone production (estrogen and progesterone), preventing your cycle from following its natural rhythm. As a result, if you've been on hormonal birth control for an extended period, your cycle may not return to its natural state immediately upon discontinuation. It can take time for your body to re-establish normal hormonal patterns, and in some cases, menstrual cycles may be irregular for months or even years after discontinuing hormonal birth control. Additionally, if you began using birth control as a teenager, your hormonal system was still maturing. During this crucial developmental phase, the use of hormonal birth control may have interfered with your body's ability to fully regulate its hormones, potentially leading to more pronounced irregularities in your cycle after discontinuation, particularly if you have been on birth control for several years.
If you want to get off of birth control:
First, congratulations on taking the step to prioritize your health! If you've been on hormonal birth control for an extended period, it's important to recognize that your body may be nutrient deficient, especially if your diet or supplementation hasn’t been properly balanced. Focus on replenishing key vitamins and minerals, particularly vitamin D, magnesium, and omega-3 fatty acids, all of which play a crucial role in hormone regulation.
Start tracking your menstrual cycle. Don’t be alarmed if the reasons you initially started using birth control (such as heavy flow, acne, or other issues) reappear. Essentially you simply just plugged your fire alarm back in and you’re reconnecting with your body, and that's something to celebrate. If you have an alarm going off, there’s a fire somewhere. Hopefully, by reading this guide, we can address and resolve some of those underlying conditions, rather than simply masking the symptoms. However, it’s important to be patient with the process and seek medical advice if problems persist. Before discontinuing birth control, you should have a clear plan in place to support your body’s transition and restore balance.
Tracking your cycle, the rhythm method:
The rhythm method is a natural form of birth control. It relies on a person tracking their fertility throughout the menstrual cycle, ensuring they do not have sex on days when they are most fertile. This method requires a person to know when they are ovulating, many women use a period tracking app but the rhythm method is a lot more reliable. Some signs a woman will track with this method is the average date of ovulation, cervical fluid, and basal body temperature (your temperature as soon as you wake up, this goes up after ovulation). The rhythm method may also: increase awareness of one’s menstrual cycle and help identify a lack of ovulation, which can be a sign of underdiagnosed conditions, such as polycystic ovary syndrome.
To get started with tracking your cycle via the rhythm method, all you need is a calendar and the date of your last period to determine your ovulation point. First, you'll want to figure out what your average cycle length is and then subtract 14. This will give you a rough estimate of the day you will begin ovulating. You ovulate once per cycle, and that egg that is released from the ovaries can only survive 12-24 hours within the reproductive tract, however experts agree that your fertile window is a bit longer and takes five days prior to ovulation along with the 24 hours that follow (that’s how longer sperm can survive vaginally). If you are using the rhythm method to avoid pregnancy, you'll want to abstain from intercourse one week before your ovulation window, along with the two to three days following. Take your temperature every morning, a slight increase in BBT (basal body temperature) that lasts for at least 3 days indicates ovulation. I included a sample of a calendar of what tracking this may look like. You can also pay attention to cervical mucus. When done correctly this method has a 99.4% effective rate. This is higher than any birth control so not only are you not subjecting your body to harm, but you are also learning and taking charge of your body which is pretty empowering.